Introduction
The menopause is a natural stage in a woman’s life, marked by the definitive cessation of menstruation. This hormonal transition is accompanied by various physiological changes such as hot flushes, mood swings, sleep disturbances, headaches, hair loss, intimate dryness… One of the most worrying is the increased risk of osteoporosis. In this article, we look at the close link between the menopause and osteoporosis by answering five key questions.
What is osteoporosis and how is it linked to the menopause?
Osteoporosis is a disease characterised by a decrease in bone density and deterioration of bone structure, making bones fragile and more likely to fracture. The menopause is a major risk factor for the development of osteoporosis, as the drop in levels of oestrogen, an essential hormone in women, plays an important role in regulating bone density.
This condition mainly affects post-menopausal women, with a prevalence two to three times higher than in men of the same age. The decline in oestrogen levels accelerates the loss of bone density, significantly increasing the risk of fractures. Unfortunately, among women aged 50 today, it is estimated that one in three or four will develop a fracture due to bone fragility during her lifetime.

Why does the menopause lead to a reduction in bone density?
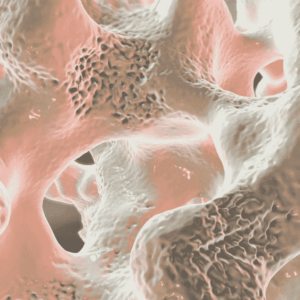
Oestrogens play a crucial role in maintaining bone health in women. During the menopause, oestrogen production falls drastically. These hormones help regulate the activity of osteoclasts, the cells responsible for bone resorption (breakdown and elimination of existing bone tissue), and encourage bone formation by osteoblasts. Estrogen deficiency upsets this balance, resulting in increased bone resorption and reduced bone formation, leading to a net decrease in bone density and increased bone fragility.
What are the additional risk factors for osteoporosis during the menopause?
In addition to reduced oestrogen levels, other risk factors can exacerbate bone loss during the menopause.
These include a family history of osteoporosis and low initial bone mass, against which nothing can be done.
Fortunately, there are others that we can do something about:
- Environmental factors
- Smoking and drinking too much alcohol: Smoking leads to a persistent state of systemic inflammation, which can have harmful effects on bone health. Smoking contributes to the early onset of the menopause and reduces the protective effect of female sex hormones during the menopause. Alcohol abuse is also harmful to bones, as it suppresses bone formation and leads to a deficiency in sex hormones.
- Eating an unbalanced diet: thinness, malnutrition or severe malnutrition are risk factors for osteoporosis, as are diets that are responsible for calcium deficiency, especially during childhood and adolescence. Excess coffee or salt can cause calcium to leak into the urine.
- Being sedentary: prolonged immobility and lack of physical activity are risk factors for osteoporosis.
Insufficient sunlight: vitamin D, synthesised by the skin thanks to the sun’s ultraviolet rays, encourages the absorption of calcium by the digestive tract.
2. Factors against which preventive measures should be taken
- Gynaecological problems: menstrual disorders, prolonged menstrual periods, spontaneous or surgical early menopause (before the age of 40); a lack of female sex hormones promotes osteoporosis.
- Having an illness or taking a treatment that favours the onset of osteoporosis: type 1 diabetes, hyperthyroidism, Crohn’s disease, rheumatoid arthritis, corticosteroid treatments (prednisone, prednisolone).
What are the symptoms of osteoporosis and how is it diagnosed?
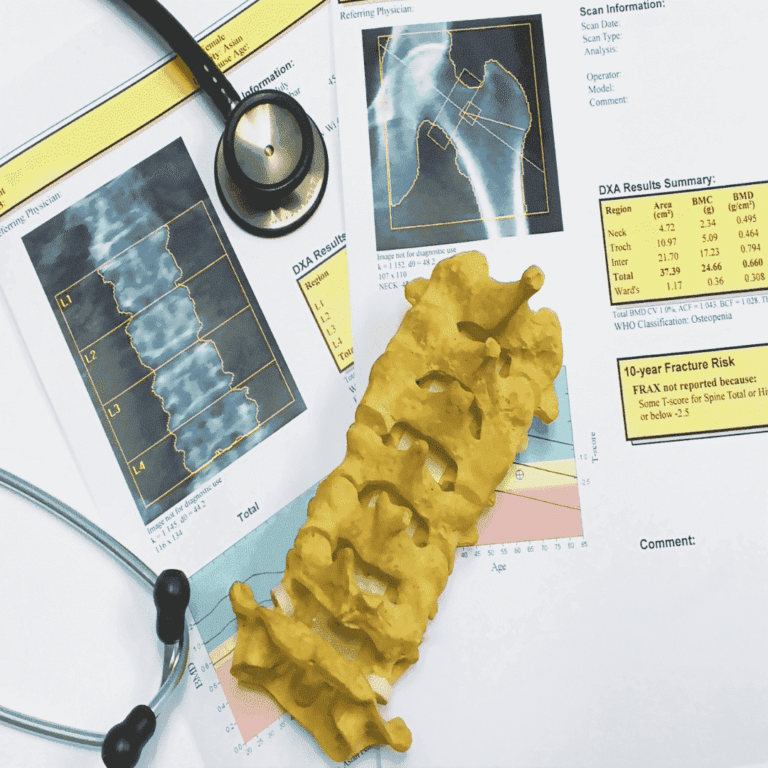
Osteoporosis is often referred to as a “silent disease” because it generally presents no specific symptoms until a fracture occurs. However, certain warning signs may include a reduction in height, stooped posture, bone pain and fractures that occur easily. Ideally, osteoporosis should be diagnosed before fractures occur. It can be confirmed by bone densitometry, a painless procedure that measures bone mineral density and serves as a benchmark for treatment. More specifically, this is a method of measuring bone density, i.e. the quantity of minerals present in the bones. This measurement is used to assess bone mass and is a valuable means of evaluating bone strength. The mineral content of the bone, mainly calcium and phosphorus, is examined during this procedure. Bone densitometry therefore provides essential information on bone health and density.
In addition, blood and urine tests are always essential to search for the cause of osteoporosis (secondary osteoporosis, i.e. osteoporosis linked to another disease, in both men and women).
How can osteoporosis be prevented and treated during the menopause?
The prevention and treatment of osteoporosis during the menopause are based on similar measures. Adopting a healthy lifestyle is essential, in particular:
- Eating a balanced diet rich in calcium and vitamin D,
- Regular physical activity,
- Stopping smoking and limiting alcohol consumption,
- Reasonable exposure to the sun.
In addition, doctors may recommend drug treatments such as bisphosphonates or selective oestrogen receptor modulators (SERMs) to prevent bone loss and reduce the risk of fractures. In addition, hormone replacement therapy, which generally includes oestrogen combined with progestins, is an effective approach for compensating for hormone deficiency and significantly reducing bone deterioration.
To conclude …
The menopause and osteoporosis are closely linked, as the decrease in oestrogen levels during the menopause contributes to increased bone loss. Understanding this link and taking preventive measures can help reduce the risk of osteoporosis and fractures in post-menopausal women. A comprehensive approach, including healthy lifestyle changes and appropriate medical treatment, can help maintain bone health and improve quality of life during and after the menopause.
Sources :
1. https://www.facebook.com/inserm.fr (no date) Ostéoporose · Inserm, La science pour la santé, Inserm. Available at: https://www.inserm.fr/dossier/osteoporose/ (Accessed: 24 July 2023).